Ulcerative proctitis is a type of inflammatory bowel disease (IBD) that specifically affects the rectum. While it may be considered a milder form of ulcerative colitis, its symptoms can still significantly affect quality of life. If you’re wondering what ulcerative proctitis is, it’s essentially a chronic inflammation of the rectal lining, which leads to discomfort, urgency, and in some cases, bleeding. Though it may not impact large portions of the colon, the condition deserves serious attention and proper treatment.
In this article, we will dive deep into the condition, discussing ulcerative proctitis causes, symptoms, treatment options, and how it compares to other forms of IBD. Additionally, we’ll explore how clinical research and trials are contributing to the future of ulcerative proctitis care.
What Is Ulcerative Proctitis?
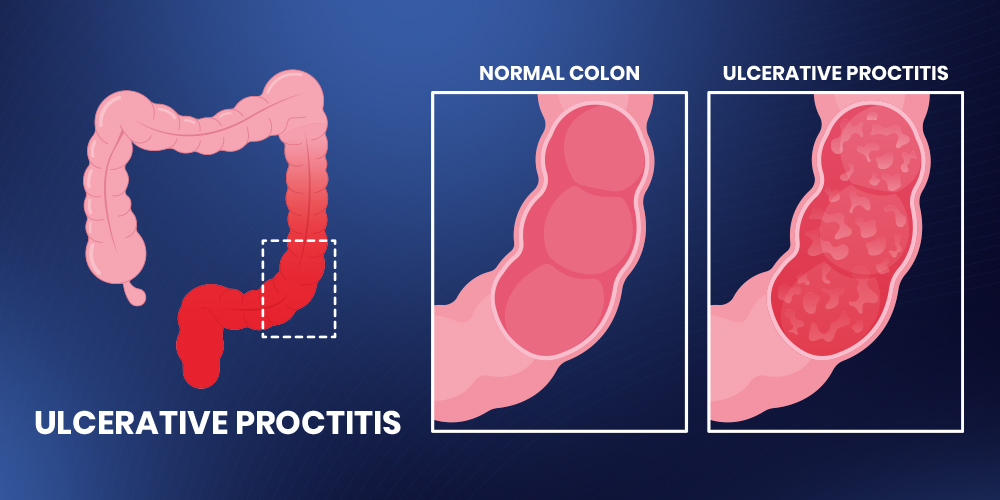
Ulcerative proctitis is an inflammatory disorder limited to the rectum, the last part of the large intestine. This condition is considered a subtype of ulcerative colitis. However, unlike more extensive forms of IBD, ulcerative proctitis involves only the rectal area. The term rectal inflammation is often used interchangeably to describe this condition.
Although less extensive than pancolitis or left-sided colitis, the swollen rectum that results from ulcerative proctitis can lead to discomfort, urgency, and rectal bleeding. Importantly, some patients experience mild symptoms while others may suffer from recurring and more severe flare-ups.
Ulcerative Proctitis Causes
Like other forms of IBD, the exact ulcerative proctitis causes remain unclear. However, medical experts believe that it results from a complex interaction of genetics, environmental factors, immune system dysfunction, and gut microbiota imbalances.
Some contributing factors include:
- Genetics: A family history of IBD increases your risk.
- Immune Response: An abnormal immune reaction may mistakenly attack the healthy tissue in the rectum.
- Environmental Triggers: Certain infections, antibiotics, or stressors may provoke inflammation.
- Diet: Although not a direct cause, diet may influence symptom severity and flare-ups.
Ulcerative Proctitis Symptoms
Recognizing ulcerative proctitis symptoms early can make a big difference in management. These symptoms typically revolve around bowel habits and rectal discomfort.
Common symptoms include:
- Rectal bleeding
- Mucus in the stool
- A feeling of incomplete bowel movements
- Frequent urge to defecate (tenesmus)
- Lower abdominal discomfort
- Mild fever during flare-ups
Since the inflammation is localized, systemic symptoms such as weight loss or fatigue are generally less prominent unless the disease progresses.
Ulcerative Proctitis vs Ulcerative Colitis
When discussing ulcerative proctitis vs ulcerative colitis, it’s crucial to understand the scope of inflammation. Ulcerative colitis affects larger portions of the colon and may extend from the rectum to other parts of the large intestine. In contrast, ulcerative proctitis is confined solely to the rectum.
Because of this difference in distribution, the treatment approach and symptom severity can vary. Patients with proctitis often experience milder symptoms, although frequent flare-ups can still be highly disruptive. On the other hand, ulcerative colitis tends to be more aggressive and systemic. Nevertheless, untreated ulcerative proctitis may evolve into a more extensive form of ulcerative colitis over time, making early intervention critical.
Ulcerative Proctitis Treatment
When it comes to ulcerative proctitis treatment, a multi-faceted approach is often required. Treatment plans depend on symptom severity, frequency of flare-ups, and individual response to medications.
1. Topical Therapy
- Mesalamine suppositories or enemas are often first-line treatments. These target the rectum directly and help reduce inflammation effectively.
2. Oral Medications
- Oral 5-aminosalicylic acids (5-ASAs) or corticosteroids may be prescribed for more persistent cases.
3. Biologic Therapies
- For patients who do not respond to conventional therapies, biologics targeting specific immune pathways may be introduced.
4. Lifestyle and Diet
- Although diet doesn’t cause the condition, it can affect flare-ups. Anti-inflammatory diets and stress management techniques can be beneficial.
Additionally, Gastroenterology Research Studies have been exploring newer biologics and non-invasive treatment options to further enhance patient outcomes.
Role of Clinical Trials in Advancing Treatment
Modern medicine owes much of its advancement to Clinical Trials for Ulcerative Colitis, many of which have yielded promising results for ulcerative proctitis as well. These trials aim to assess the efficacy and safety of emerging therapies under strict clinical trials safety regulations.
Clinical Trial Recruitment
Clinical Trial Recruitment plays a vital role in developing new therapies. Volunteers not only gain early access to cutting-edge treatments but also contribute significantly to science and future care models.
Numerous trials are currently underway that investigate oral biologics, microbiome-based treatments, and even personalized immunotherapy. These trials are monitored by Clinical Investigators and often backed by top institutions, ensuring participant safety and regulatory compliance.
The Importance of Early Diagnosis and Monitoring
Early diagnosis helps to prevent disease progression and improves quality of life. Physicians may use a combination of sigmoidoscopy, stool tests, and biopsies to confirm diagnosis. Continuous monitoring allows for timely interventions, which is particularly important in managing recurring flare-ups and minimizing rectal damage.
In recent years, research has also focused on the gut-brain connection in ulcerative proctitis, suggesting that mental health can influence disease activity. Anxiety and depression are common among IBD patients, and managing these conditions through therapy or mindfulness can lead to better outcomes. Furthermore, advancements in non-invasive diagnostic tools, such as fecal calprotectin tests, offer promise for early detection of inflammation. As public awareness grows, patients are increasingly seeking second opinions and exploring clinical trials for ulcerative colitis, even when only the rectum is involved. Ultimately, an individualized care plan remains the cornerstone of effective ulcerative proctitis treatment.
Conclusion
In summary, ulcerative proctitis is a manageable but often misunderstood condition. While it may not affect as large an area as ulcerative colitis, the symptoms can still interfere with daily life. Fortunately, through proper treatment, lifestyle adjustments, and participation in Gastroenterology Research Studies, many patients achieve long periods of remission.
If you or someone you know is struggling with rectal discomfort or bleeding, don’t delay medical evaluation. Prompt diagnosis and treatment can significantly improve outcomes, and you may even consider enrolling in a clinical trial to access cutting-edge therapies under the supervision of trained Clinical Investigators. By staying informed and proactive, patients with ulcerative proctitis can lead healthy, fulfilling lives.
Frequently Asked Questions
Is proctitis worse than ulcerative colitis?
Not necessarily. Ulcerative proctitis is generally considered less severe than ulcerative colitis because it affects a smaller area (only the rectum). However, frequent flare-ups and untreated inflammation can significantly affect quality of life and may evolve into more extensive disease over time.
How do you treat a proctitis flare-up?
A proctitis flare-up is typically managed with increased use of topical medications such as mesalamine suppositories or enemas. In more severe cases, oral corticosteroids or biologic drugs may be needed. Stress management and diet modification can also help control symptoms during a flare.
What causes ulcerative proctitis flare-ups?
Flare-ups may be triggered by stress, infections, dietary changes, medication non-compliance, or unknown immune reactions. Sometimes, even minor disruptions to gut balance can provoke renewed inflammation in the rectum.
Does ulcerative proctitis ever go away?
While ulcerative proctitis is a chronic condition and technically doesn’t “go away,” many patients achieve long-term remission with proper treatment. Some individuals experience few or no symptoms for extended periods, especially when adhering to prescribed therapy and lifestyle measures.


