Key Points:
- Psoriatic arthritis is an autoimmune condition affecting joints and skin simultaneously
- Symptoms range from mild joint pain to severe inflammatory damage
- Early diagnosis and treatment prevent long-term joint damage
- Understanding your condition empowers better health decisions
Understanding Psoriatic Arthritis
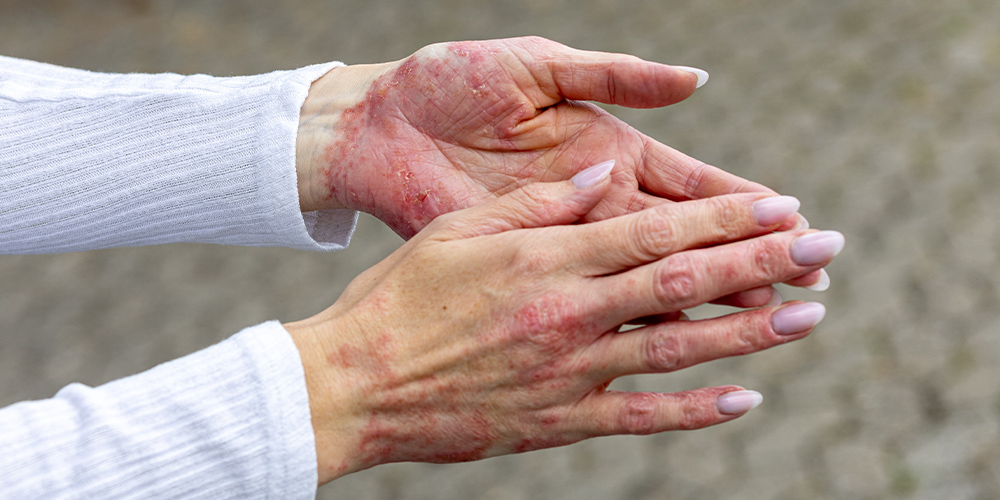
You wake up with swollen fingers and painful knees. Your skin shows red, scaly patches. These symptoms might seem unrelated, but they could point to psoriatic arthritis.
This condition combines joint inflammation with psoriasis skin disease. Understanding psoriatic arthritis changes how you approach your health.
This blog explains what causes joint pain with psoriasis. Furthermore, you’ll discover treatment options that improve your quality of life. Knowledge helps you take control of your health journey.
What is Psoriatic Arthritis? A Clear Definition
Psoriatic arthritis is an autoimmune inflammatory arthritis linked to psoriasis. Your immune system mistakenly attacks joint tissues and skin cells. This creates inflammation in your joints and skin simultaneously.
The condition affects roughly one in every 100 people with psoriasis. Additionally, about 30 percent of psoriasis patients develop arthritis. You can still have arthritis even if skin symptoms are mild. Some people experience joint pain before any skin involvement appears. Early recognition helps prevent permanent joint damage.
Can Psoriasis Cause Joint Pain?
Many people wonder whether psoriasis directly causes joint pain. When your body’s defense system malfunctions, it attacks healthy tissues.
In psoriasis, immune cells target skin cells excessively. In psoriatic arthritis, these same immune cells attack joint tissues. Consequently, both conditions often occur in the same person.
How Psoriasis and Joint Disease Link
Your immune system produces inflammatory molecules called cytokines. These chemicals trigger inflammation in your skin and joints. Additionally, specific genetic factors make some people vulnerable. Furthermore, environmental triggers can activate this immune response.
The inflammation damages cartilage and bone over time. This is why early treatment matters significantly. Your healthcare provider can test for inflammatory markers confirming psoriatic arthritis.
When Joint Symptoms Develop
Joint symptoms can appear at different times in your disease journey. For some patients, arthritis develops years after psoriasis appears. For others, joint pain comes first, followed by skin symptoms.
Some people experience both conditions simultaneously from the start. The timing varies based on your genetics and environmental exposures.
Roughly 10 percent of people develop arthritis before any skin symptoms. So, if you have psoriasis and joint pain, see a rheumatology specialist.
Signs of Psoriatic Arthritis: What You Need to Know
Recognizing early symptoms helps you get timely treatment. Psoriatic arthritis presents differently from other arthritis types. Some signs appear in your joints, while others affect your entire body.
Joint Symptoms and Pain Patterns
Joint pain and swelling are the hallmark signs. Your fingers, toes, wrists, and knees are commonly affected. Additionally, pain often affects both sides of your body equally. Stiffness in the morning is a typical early warning sign.
Furthermore, pain may worsen with activity or improve with rest. Consequently, your joints may feel warm and tender. Pain can range from mild discomfort to severe, limiting movement. Moreover, some people develop asymmetrical arthritis affecting only one side.
Skin, Nail, and Systemic Symptoms
Beyond joint pain, psoriatic arthritis affects other body systems. Your skin shows red, scaly patches typical of psoriasis. These appear on elbows, knees, scalp, and palms. Additionally, your nails may become pitted, discolored, or thickened. Nail involvement is unique to psoriatic arthritis among arthritis types.
Furthermore, some people experience eye inflammation and fatigue. Fatigue can be severe and affect daily functioning. Consequently, patients often report low energy levels. Your healthcare team should address all symptoms, not just joint pain.
What Causes Psoriatic Arthritis? Genetic and Environmental Factors
Multiple factors work together to cause psoriatic arthritis. No single cause explains why this condition develops. Instead, genetics and environment interact in complex ways.
Genetic History
Your genes significantly influence psoriatic arthritis risk. Certain genetic variations increase vulnerability to this disease. Having a family history of psoriasis or arthritis increases your risk.
Environmental factors must also be present to trigger disease development. Your genes load the gun, but environment pulls the trigger.
Environmental Triggers and Risk Factors
Environmental factors can activate psoriatic arthritis in genetically susceptible people. Infections, particularly streptococcal infections, are known triggers. Additionally, physical trauma or injury to joints can initiate symptoms. Stress plays a significant role in disease flares for many patients.
Furthermore, skin injuries can trigger both psoriasis and arthritis symptoms. Smoking increases your risk of developing psoriatic arthritis significantly. Additionally, poor diet and obesity may worsen inflammation. Consequently, lifestyle changes can help manage your condition effectively.
How Is Psoriatic Arthritis Diagnosed?
Diagnosing psoriatic arthritis requires a thorough evaluation by specialists. No single test confirms this diagnosis definitively. Instead, doctors combine physical exams, blood tests, and imaging studies. Early diagnosis prevents joint damage, so seek evaluation if symptoms persist.
Your rheumatology specialist starts with a detailed medical history. They ask about joint pain, skin symptoms, and family history. Furthermore, they perform a physical examination of your joints and skin. They look for swelling, tenderness, and warmth in your joints. Additionally, doctors assess your range of motion and joint function.
Blood tests measure inflammatory markers like ESR and CRP. Furthermore, doctors check for rheumatoid factor and anti-CCP antibodies. You’ll test negative for these in psoriatic arthritis, unlike rheumatoid arthritis. Imaging studies like X-rays show joint damage patterns.
Additionally, ultrasound and MRI provide detailed views of inflammation. Consequently, your doctor combines all this information to make a diagnosis. The CASPAR classification criteria help confirm psoriatic arthritis diagnosis. Early detection allows your team to start treatment immediately.
Rheumatoid Arthritis Clinical Trials
Access Research-Based Treatment Options for Rheumatoid Arthritis
Clinical trials may provide access to investigational therapies aimed at reducing inflammation and improving joint function.
Distinguishing Psoriatic Arthritis from Rheumatoid Arthritis
Psoriatic arthritis and rheumatoid arthritis seem similar but differ importantly. Understanding these differences helps guide your treatment decisions. Your healthcare provider must distinguish between these conditions accurately.
What is Rheumatoid Arthritis?
Rheumatoid arthritis is an autoimmune disease affecting your joints. Unlike psoriatic arthritis, it doesn’t involve skin inflammation. It typically affects both sides of your body symmetrically. Rheumatoid arthritis usually targets smaller joints like fingers and wrists. Additionally, it causes morning stiffness lasting more than one hour. Consequently, treatment approaches differ from psoriatic arthritis management. Your doctor must determine which condition you have for proper treatment.
Read more: Osteoarthritis vs Rheumatoid Arthritis: A Complete Guide
Seropositive vs. Seronegative Rheumatoid Arthritis
Rheumatoid arthritis is classified into two major types based on blood tests. Seropositive rheumatoid arthritis means your blood contains rheumatoid factor antibodies. Additionally, you test positive for anti-CCP antibodies. Furthermore, seropositive disease typically causes more severe joint damage. Patients with seropositive disease often need aggressive treatment early.
Seronegative rheumatoid arthritis means you test negative for these antibodies. However, you still have rheumatoid arthritis based on symptoms and imaging. Furthermore, seronegative disease often progresses more slowly than seropositive. Additionally, some seronegative patients have fewer joint complications. However, early treatment remains important for both types. Psoriatic arthritis patients always test negative for rheumatoid factor. This key difference helps doctors distinguish between these arthritis types.
Also read: How is Seronegative Rheumatoid Arthritis Diagnosed: A Patient’s Guide
Comparing Arthritis Types and Key Features
| Feature | Psoriatic Arthritis | Seropositive RA | Seronegative RA |
|---|---|---|---|
| Typical Onset | Age 30–50 with psoriasis | Age 40–60, any gender | Age 40–60, any gender |
| Joints Affected | Fingers, toes, spine, knees | Small joints (symmetric) | Small joints (symmetric) |
| Skin Involvement | Yes, psoriasis patches | No skin involvement | No skin involvement |
| RF Factor | Negative | Positive | Negative |
| Anti-CCP | Negative | Positive | Negative |
| Morning Stiffness | 30–60 minutes | 1+ hours | 30–60 minutes |
| Nail Involvement | Yes, pitting and discoloration | No involvement | No involvement |
| Treatment Approach | DMARDs, biologics, TNF inhibitors | Aggressive early treatment | Moderate early treatment |
| Prognosis | Variable, joint damage preventable | More severe if untreated | Generally slower progression |
Psoriatic Arthritis Treatment Options: From Medication to Clinical Trials
Multiple treatment approaches help manage psoriatic arthritis effectively. Your healthcare team creates a personalized treatment plan based on severity. Early intervention prevents permanent joint damage and disability.
Conventional Therapies and Biological Medications
NSAIDs reduce pain and inflammation in mild cases. However, they don’t prevent progressive joint damage. Consequently, doctors often recommend disease-modifying antirheumatic drugs (DMARDs). Methotrexate is a commonly prescribed DMARD for psoriatic arthritis. Additionally, biologic medications target specific immune molecules causing inflammation.
TNF inhibitors like etanercept and infliximab work very effectively. Furthermore, IL-17 inhibitors represent newer biologic options. Many patients respond better to biologic therapies than conventional DMARDs. Your rheumatology team monitors your response and adjusts treatment accordingly. Combination therapy often works better than single medications.
Why Clinical Trials Matter for New Treatments
Clinical trials test innovative treatments before they become available. Consequently, trial participants access cutting-edge therapies early. Furthermore, you contribute to medical knowledge that helps future patients. Clinical research has led to remarkable improvements in psoriatic arthritis care. New biologic medications continue to emerge from rigorous clinical studies.
Moreover, clinical trials closely monitor your safety throughout participation. Your healthcare rights are protected by strict safety regulations. Clinical trials in Massachusetts offer opportunities to participate in advanced research. If you’ve failed standard treatments, clinical trials may offer hope. Your rheumatology team can determine if you qualify for current studies.
Living With Psoriatic Arthritis
Daily management strategies help you maintain function and quality of life. Working with your healthcare team ensures comprehensive care addressing all symptoms. Additionally, lifestyle modifications significantly impact disease progression.
Furthermore, regular physical activity strengthens muscles supporting your joints. Low-impact exercises like swimming and walking reduce stress on joints. Additionally, physical therapy improves flexibility and range of motion. Proper nutrition reduces inflammation and supports joint health. Furthermore, foods rich in omega-3 fatty acids help control inflammation. Managing stress through meditation and counseling improves disease outcomes.
Additionally, adequate sleep supports your immune system function. Moreover, protecting your joints prevents injury and reduces pain. Your rheumatology team can recommend specific strategies for your situation. Regular follow-up appointments help catch complications early. Consequently, consistent communication with your healthcare provider improves outcomes significantly.
Rheumatology Clinical Trials at Lucida: Advancing Psoriatic Arthritis Care
Lucida Clinical Trials leads innovation in rheumatology research. Our commitment focuses on advancing treatment options for psoriatic arthritis. Furthermore, we conduct rigorous clinical research studies testing new medications. Our clinical trials in Massachusetts recruit patients seeking better outcomes. We offer access to novel biologic therapies and combination treatments.
Additionally, our team monitors safety throughout your participation carefully. Our clinical trials safety regulations exceed industry standards. Participant protection remains our highest priority always. Many patients have benefited from accessing new treatments through our programs. If standard treatments haven’t worked well, clinical trials may offer hope. Furthermore, your participation contributes to medical knowledge benefiting countless future patients. Contact our research team to learn if you qualify for current opportunities.
Rheumatoid Arthritis Clinical Trials
Access Research-Based Treatment Options for Rheumatoid Arthritis
Clinical trials may provide access to investigational therapies aimed at reducing inflammation and improving joint function.
Conclusion:
Psoriatic arthritis combines joint pain with skin inflammation. Early recognition and treatment prevent permanent damage. Furthermore, multiple effective medications can control your symptoms. Understanding your condition empowers you to make informed decisions. Additionally, working with specialists ensures you receive proper care. Moreover, clinical trials offer access to innovative new treatments.
Don’t delay seeking evaluation if you experience joint pain with psoriasis. Furthermore, ask your rheumatology team about clinical trial opportunities. Your involvement in research advances care for everyone. Together, we can improve outcomes and quality of life. Contact Lucida Clinical Trials today to learn more about our active research studies. Your better health starts with taking action now.
Frequently Asked Questions
Is psoriatic arthritis an autoimmune disease?
Yes, psoriatic arthritis is definitely an autoimmune disease. Your immune system attacks healthy joint tissues and skin cells. This causes inflammation and tissue damage over time. Early treatment prevents serious complications.
How to treat psoriatic arthritis?
Treatment combines medications, physical therapy, and lifestyle modifications. DMARDs and biologic medications reduce inflammation. Furthermore, physical activity and stress management support your treatment plan. Additionally, clinical trials offer access to newer treatment options.
Is psoriatic arthritis a rare disease?
No, psoriatic arthritis affects roughly one in every 100 people. Additionally, about 30 percent of psoriasis patients develop arthritis. It’s more common than many people realize, yet often diagnosed late.
Can it be cured?
Currently, psoriatic arthritis cannot be cured, but it can be managed effectively. Early treatment prevents joint damage and maintains function. Many patients achieve remission or low disease activity with proper care. Clinical research continues advancing toward better treatment options.